I have a disease called Ulcerative Colitis. Do genes cause my disease?
June 25, 2009

- Related Topics:
- Complex traits,
- Autoimmune disease,
- Environmental influence,
- Medical genetics
An elementary school teacher from California asks:
“I have a disease called Ulcerative Colitis. Do genes cause my disease?”
Genes seem to be involved in increasing someone's risks for getting ulcerative colitis (UC). But they are not the whole story. Where you live, what you eat, and what's around you plays an important role, too.
Ulcerative Colitis is a Disease of the Large Intestine
UC is a disease that affects your large intestine. Your large intestine is a long tube of cells that soaks up water and nutrients from the food you eat. It is also home to as many as 500 different kinds of helpful bacteria that help us process our food1.
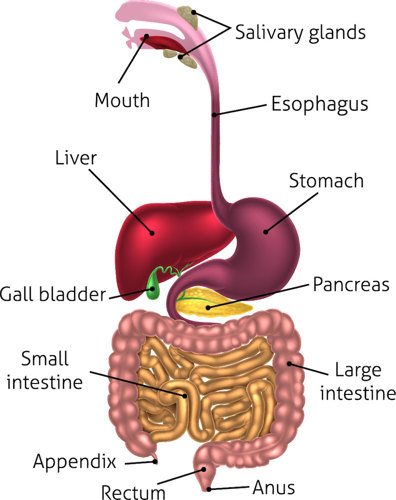
A person who has UC gets sores in the walls of their large intestine. They also tend to lose many of the helpful bacteria that usually live there.
Both of these things happen because the patient's immune system gets confused. Normally an immune system recognizes and attacks foreign invaders like bad bacteria and viruses. The immune systems of people with UC think that the wall of the large intestine and some of the good bacteria that live there are invaders2.
So the immune system attacks these things. And this causes the sores on the walls of the large intestine. This also causes problems like bleeding and diarrhea. As you can imagine, people with UC don't digest their food or absorb nutrients as well as the rest of us. And this can be very dangerous.
Ulcerative Colitis is Partly Genetic
Scientists have classified UC as a genetic disease. So what's the evidence?
First, UC can run in families. If you have a close relative with the disease, the chances of you also getting it are as high as 15%. If no one in your family has the disease, your chances are about 1%. So you are 15 times more likely to get UC if someone in your family already has it3. But these facts aren't as convincing as they seem.
The reason is that families tend to live all in the same place and are exposed to the same things. So if something in your environment is making you sick, chances are it will also make the people around you sick too. Imagine that a family paints their house with lead paint. Chances are that some of the people living in that house will get sick. But this doesn't mean that the sickness runs in the family. It just means that they were all exposed to lead.

One way that scientists can figure out if a disease is genetic is by doing twin studies. There are two kinds of twins: fraternal and identical. Identical twins have nearly identical copies of their DNA. That's why they look so much alike. Fraternal twins only share about half of their DNA, which is about the same as any brother or sister.
If both twins in an identical twin pair get a disease more often than both fraternal twins in a pair, then genes are most likely important. If they all get the disease at about the same rate, then the environment is important.
Scientists have found that both twins in an identical twin pair have UC about 18% of the time. Both twins in a fraternal pair only get the disease about 4.5% of the time. The difference between 4.5% for fraternal twins and 18% for identical twins tells us that genes are important in causing UC4.
The specific genes that contribute to UC are still a mystery. Scientists think that there are different ways to get UC. And that each way may use a different set of genes. So far, scientists have found at least 12 different regions in our DNA that might contribute to someone getting UC*. Scientists are working hard to figure out why these regions are important, but there is still a lot of work to be done2,5.
This is a common problem for a lot of other diseases, too. It's not always easy to understand what genes cause a disease, especially if there are lots of genes involved.
The Environment Plays a Big Role in Ulcerative Colitis
But genes aren't the only thing that can cause UC. How do we know that? Think back to the identical twin study. If genes were the only cause of UC, then if one identical twin had the disease, then the other twin would also have it 100% of the time. Because they have the exact same genes.
This clearly isn't the case here. Around 82% of the time, only one identical twin has UC. This means that there is definitely something else that contributes to whether you will get the disease.
That something else is the environment that we live in. Some diseases need certain triggers from the environment to make you sick. In these cases, your genes can make you more sensitive to these triggers. And if you are more sensitive to the triggers, you are more likely to get the disease.
UC appears to be one of these diseases. Scientists are working hard trying to find these triggers2. So far, though, they haven't been too successful.
Scientists have found, for example, that people who have UC are more likely to live in a city than in the country. MigrantsImmigrants who move to a more crowded city from somewhere less crowded also have a higher chance of developing the disease6,7. It's hard to know what exact thing about cities makes us more likely to get UC. It might be more toxins in the air we breathe, exposure to more germs, more stress, or lots of other possibilities2.
Scientists have also found that diets high in fats and sugars, smoking, and some kinds of infections can also affect your chances of getting ulcerative colitis2. And I am sure they will find more triggers as well.
Conclusion
Scientists are still trying to understand how all of these things can fit together to make you sick. As you can see, lots of factors work together to give you UC. The genes you get from your family and the environment that you live in are all very important.
* Editor’s Note (4/25/2022): Genome-Wide Association Studies (GWAS) have now identified 163 regions of the DNA that affect a person’s chances of getting UC. However, these regions only collectively explain 4.1% of the variance in disease risk8. So, while UC is partially a genetic disease, environmental factors play a larger role. Smoking, having an appendectomy, and maternal breastfeeding reduce the risk for UC, while perinatal infections, measles infections and oral birth control use increase the risk for UC9.

Author: Stacey Wirt
When this answer was published in 2009, Stacey was a Ph.D. candidate in the Department of Cancer Biology, studying regulation of cell cycle and differentiation in embryonic stem cells in Julien Sage's laboratory. Stacey wrote this answer while participating in the Stanford at The Tech program.
 Skip Navigation
Skip Navigation
