Does blood type matter for pregnancy?
March 24, 2020

- Related Topics:
- Blood type,
- ABO blood type,
- Rh factor,
- Reproduction
A graduate student from Nepal asks:
“Does blood group matter in procreating baby? If yes, can you tell me with which group combination you cannot make?”
Usually, we don’t have to worry about blood type when deciding to have a child.
However, there are some exceptions. In particular, an Rh negative mother can sometimes have pregnancy complications - though doctors have an easy way to fix this issue!
Blood Type
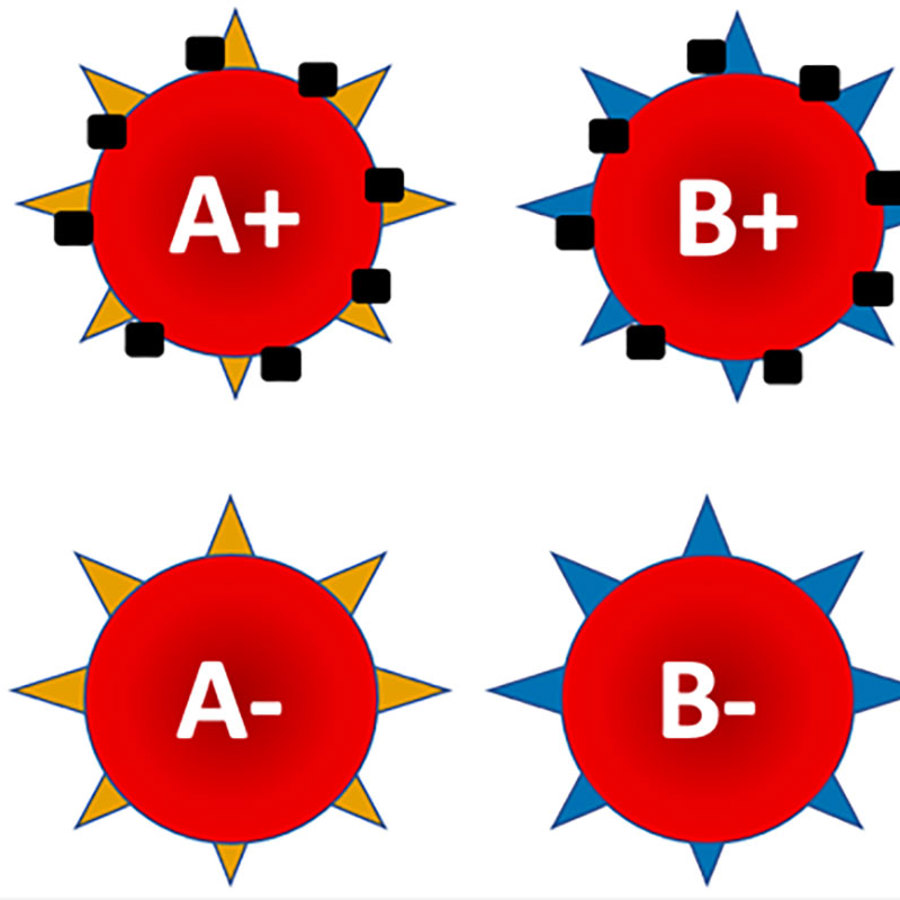
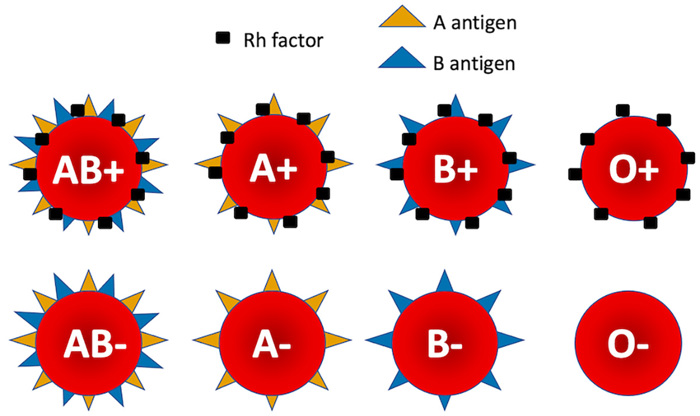
There are 8 main blood types: A+, A-, B+, B-, AB+, AB-, O+, or O-.
A person’s blood type is determined based on the decorations that surround their blood cells. There are two main blood groups:
- ABO blood group
- Rhesus factor (Rh)
For more on how these are inherited, see this article on ABO type or this article on Rh type.
Usually when planning to have a child, the doctor will take a look at the blood groups of both parents to decide if there’s any risk during the pregnancy. Usually there’s nothing to be worried about, though a few exceptions are talked about below.
Rh Incompatibility in Pregnancy
Problems can occur when the mother is Rh- and the baby is Rh+. This mismatch in blood type is often referred to as Rh incompatibility.
This mismatch doesn’t cause any problems for the first pregnancy. But it can lead to problems in later pregnancies.
During birth, the blood of mother and baby will mix. In a mom that is Rh-, her immune system won’t recognize the Rh+ in the baby’s blood. The mom’s immune system will think these definitely don’t belong – her own blood cells don’t have Rh!
Later after birth, the Rh- mom’s immune system will create antibodies that will attack any Rh+ blood they see in the future. It takes some time for the mom to make these antibodies, so these antibodies are not usually an issue during the first pregnancy.
But in future pregnancies, if the mom’s immune system sees any Rh proteins, they are treated like foreign invaders! It will attack any Rh+ blood cells, even those of the mom’s own unborn baby. This is referred to as Rh disease of the newborn.
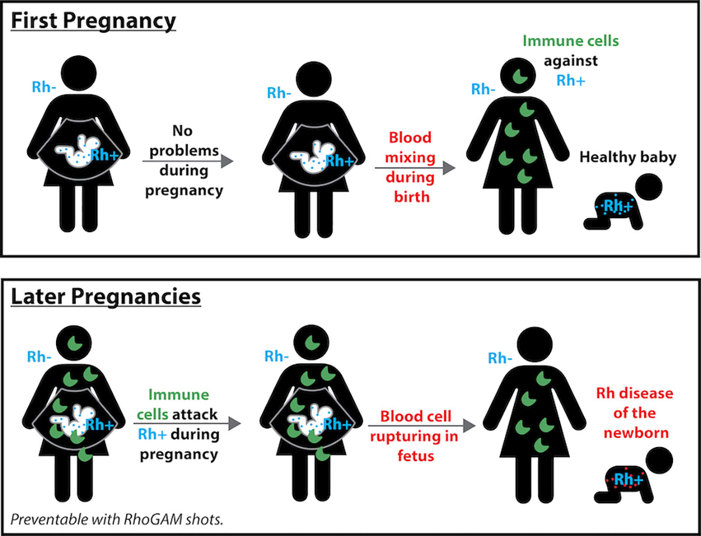
Luckily, the medical community found a solution to this back in the 1960s. If there is a risk of Rh incompatibility, doctors will give a series of RhoGAM shots during pregnancy. The first one is given around the 28th week of pregnancy, and another just after birth.
These shots prevent the mother's immune system from harming the baby. Basically, the RhoGAM absorbs all the Rh+ cells released from the baby. Without these cells present, the mom’s immune system won’t develop the antibodies that attack the baby’s blood cells. Now the unborn baby’s blood cells are protected.
With RhoGAM, we don’t have to worry about Rh incompatibility during pregnancy anymore.
ABO Incompatibility in Pregnancy
Unlike Rh incompatibility, ABO incompatibility during pregnancy is rarely a problem -- even when the mother’s ABO group doesn’t match the baby’s ABO group!
In situations where a mother has Type O blood, and the baby has A, B, or AB blood, the mother’s immune system will recognize the baby’s blood as foreign. The mother’s immune system will then create special antibodies that attack the ABO group of the baby’s blood cells, just like in Rh incompatibility.
But these antibodies are different than the antibodies that attack the Rh proteins!
These ABO group antibodies are too large to cross the placental barrier and get into the baby’s blood. If they can’t get into the baby’s blood, then there’s no way for them to attack the unborn baby.
Problems from ABO incompatibility will occur only after the delivery. And even in the uncommon deliveries where it is a problem, doctors can administer a blood transfusion. While this may sound scary, it is a routine medical procedure where the doctors add more blood to your body to make you healthy!
Conclusion
It’s always important to see a doctor before having a baby! Even in cases where blood group incompatibility is a problem, a doctor can help you to figure out the best plan forward to keep you and your baby happy and healthy.
![]()

Author: Rebecca Culver
When this answer was published in 2020, Rebecca was a Ph.D. candidate in the Department of Genetics, studying bacteria in the gut microbiome in KC Huang's laboratory. She wrote this answer while participating in the Stanford at The Tech program.
 Skip Navigation
Skip Navigation
