
My daughter lost a pregnancy due to Trisomy 18. What are the chances it could happen again?
June 6, 2012

- Related Topics:
- Trisomy/Aneuploidy,
- Meiosis,
- Chromosomes,
- Reproduction,
- Medical genetics,
- Mosaicism,
- Translocation
A curious adult from Oregon asks:
I am sorry to hear about your daughter’s miscarriage. Without having more information, I can’t give an estimate of the chances that Trisomy 18 might happen again. It is important to talk with your doctor or a genetic counselor who can give you advice about your specific situation.
What I can say is that most trisomies like this are totally random, so one trisomy pregnancy does not always mean that there is a much higher risk of a second one. That being said, some studies have found that people who have had a trisomy pregnancy may be at a slightly higher risk of a second trisomy pregnancy later on.1 The risk of having a second Trisomy 18 pregnancy is estimated to be around 1%.2
Also, a woman’s chances for a trisomy pregnancy mostly depend on her age.
For example, a 25 year old mother has around a 1 in 10,000 chance of having a Trisomy 18 pregnancy. At 45 years old, that risk goes up to 50 in 10,000.3
What I want to do for the rest of this article is focus on what trisomies are and how they happen. Then I’ll end with some of the ways that you can have an increased risk for having a trisomy pregnancy.
Trisomy Means an Extra Chromosome
Chromosomes are structures in our cells that hold our DNA or genetic information. Normally a person has 23 pairs of chromosomes, or 46 individual chromosomes, in each of their cells. Half are inherited from one parent, and half from the other, so each parent gives their baby 23 chromosomes.
Pairs of chromosomes are numbered 1 through 22, and the 23rd pair is named “X” and “Y”. Chromosomes are numbered based on their size, with chromosome 1 being the largest and chromosome 21 the smallest.
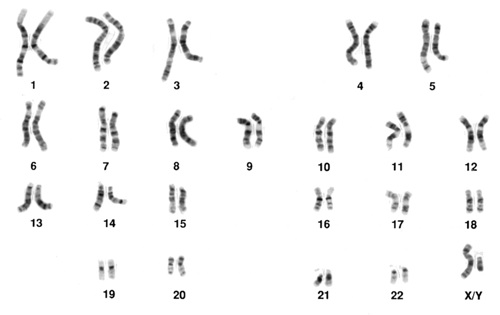
Trisomy 18 means that a person has three copies of chromosome number 18, instead of two (the “tri” in “trisomy” indicates a third chromosome). This extra chromosome causes severe developmental problems, and most Trisomy 18 pregnancies will end in miscarriage.4 Most babies born with Trisomy 18 will not survive longer than one year.2
Chromosomes Divide
Egg and sperm cells each have 23 chromosomes, or half of a full set. During fertilization, they combine their chromosomes to make a full set of 46. To make eggs or sperm with half the normal number of chromosomes, cells need to go through a complicated process called meiosis, which is illustrated below:
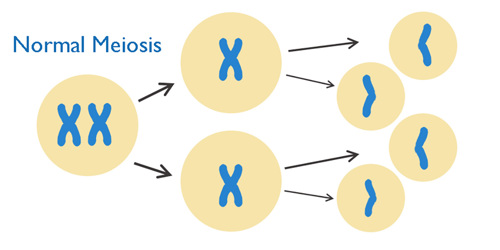
The starting cell has one pair of chromosomes, which have been duplicated. The cell divides into two cells that each have one duplicated chromosome, and then each of these cells divides again, splitting the duplicated chromosomes into single chromosomes.
The final result is four cells that each have a single chromosome. This happens for all 23 pairs of chromosomes, so the final egg or sperm cells only have 23 individual chromosomes, instead of 23 pairs.
However, sometimes meiosis goes wrong and a cell can end up with an extra or missing chromosome.
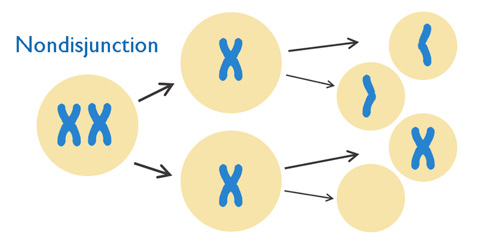
If you look at this picture you can see that one chromosome did not separate the way it should have. This means that one cell now has an extra copy of the chromosome, while the other cell has no copies. This is called “nondisjunction.”
When something like this happens, a person passes an extra chromosome onto their baby, and the baby will have 3 copies of that chromosome, or a trisomy. If the chromosome is number 18, then the baby will have Trisomy 18.
This can also happen with other chromosomes. For example, if this happens with chromosome 21, then a baby will have Trisomy 21, or Down’s Syndrome.
Figuring Out Your Risk
There are many factors that can affect a woman’s chances of having a trisomy pregnancy. As I said in the introduction, the key factor is age. The older a person is, the more likely it is that nondisjunction will happen.
For most women, age is the main risk factor. But a few women will be at a higher risk because they are having trisomy pregnancies for a different reason than nondisjunction. Luckily these are not very common.
I won’t have time to go into a lot of detail on all these special cases, but what I can do is list a few and how common they are.
Mosaicism
Although it’s rare,some people have cells in their body that carry the wrong number of chromosomes without knowing it. This is called “mosaicism,” and can lead to an increased risk of multiple trisomy pregnancies.5
If a person has a small fraction of cells in their body that carry a trisomy, they might not show symptoms. But if some of their sperm or egg cells carry the trisomy, they can pass on the extra chromosome to their children. Also, some people may have “germline mosaicism,” meaning they have the wrong number of chromosomes in their sperm or egg cells, but not in other cells of their bodies.
Mosaicism can increase the chances of having another child with a trisomy since a rare, random, nondisjunction event doesn’t have to happen. The eggs or sperm are “preloaded” with the extra chromosome.
Balanced Translocation
Around 0.2% of the population has a balanced translocation.6 This has no effect on the person but increases the risk for a trisomy pregnancy. They basically have two of their chromosomes stuck together. This causes the two chromosomes to travel together when a sperm or egg is made. The risk of having a trisomy pregnancy can be much higher for a parent who carries a balanced translocation.
So, as you can see there is not a simple answer. This is why it is so important to see a genetic counselor to figure out if you are at a higher risk of a trisomy pregnancy based on your genetics and family history.

Author: Nadine Rayes
When this answer was published in 2012, Nadine was a student in the Stanford MS Program in Human Genetics and Genetic Counseling. Nadine wrote this answer while participating in the Stanford at The Tech program.
 Skip Navigation
Skip Navigation
